- HOME
- VENUE
- RSVP
- REGISTRY
- CONTACT
- George carlin youtube comments
- Free avast or avg free bestfor vista
- Glary utilities reddit
- How to find better gifs on facebook messenger
- Best price for turbotax premium 2017
- Create image of hard drive windows vista
- Stean unlocked cities skylines all dlc
- Sekirei crossover fanfiction
- What is turbo boost macbook
- Depression dsm 5
- Install apache spark ubuntu
- Mount and blade warband mods download
- Official filmora video editor free download for windows mac
- Is driveridentifier legit
- How to upload a youtube video with beaver builder
- Lil bow wow and omarion songs
- Best mouse for macbook pro 13

This should be observed by others and not just something the patient feels. Psychomotor agitation (restless symptoms, inability to sit still, pacing, handwringing) or retardation (slowing down of thoughts, actions or speech) almost every day.
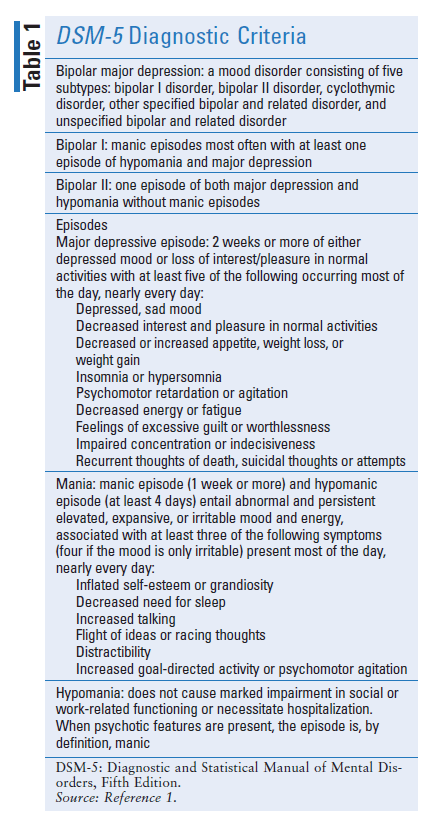
At least one of the symptoms needs to be a depressed mood or loss of interest or pleasure. The patient must have had five or more of the symptoms listed below and these must have been present during the same two-week period and be a change from previous functioning.To diagnose depression (major depressive disorder), the following DSM-5 criteria need to be met: The DSM-5 is described as a ‘companion’ publication to the World Health Organization’s (WHOs) system for International Statistical Classification of Diseases and Related Health Problems (ICD). More accurate definitions of the various disorders are also expected to help researchers in their efforts to develop drug therapies and other interventions.
DEPRESSION DSM 5 UPDATE
This latest update to the DSM is expected to especially help people whose symptoms aren’t well defined and don’t fit neatly with the old criteria outlined in the DSM IV, making it difficult for them to get a diagnosis and help. The American Psychiatric Association (APA) took almost a decade to prepare the DSM-5, which was a long process involving the input of more than 100 researchers and clinicians in the areas of mental disorders and related fields. The DSM-5 provides a much needed update to the classification system used for mental disorders and was published on May 18, 2013.
DEPRESSION DSM 5 MANUAL
It does not include treatment guidelines.ĭSM-5 is the fifth and latest version of the Diagnostic and Statistical Manual of Mental Disorders, which was first published in 1952. It includes descriptions, symptoms and further criteria that help accurately define and characterize mental disorders. This gives me the feeling that depression may become overdiagnosed and anti-depressants overprescribed for what should be ‘normal’ grief.DSM-5 (DSM V) is a handbook that lists the criteria for assessing and diagnosing mental disorders. In removing the ‘bereavement exclusion’, the DSM-5 encourages clinicians to diagnose major depression in persons with normal symptoms of bereavement after only 2 weeks of mild depressive symptoms. The 5th edition of the DSM , which is due out this year, would characterize bereavement as a depressive disorder.

“Grief is not a disorder and should be considered normal even if it is accompanied by some of the same symptoms seen in depression.” – Eric Widera, Geriatrician But, researchers have noted, grief rarely produces the symptoms of depression, such as low self-esteem or feelings of worthlessness. Those suffering from grief report symptoms that are also symptoms of major depression sadness, tearfulness, insomnia and decreased appetite. Grief usually runs its course within 2-6 months and typically does not require treatment with medications. When one’s health suffers and they lose friends and loved ones, the sentiment went, why wouldn’t they be depressed? The DSM-IV clearly distinguishes between normal and expected grief after loss from the more persistent and severe symptoms of clinical depression. As one who works with older adults, I have experienced the reality for many older adults, after a certain age it is more likely, that one is faced with death on a regular basis.ĭepression has been underdiagnosed in older adults.

Grief/Bereavement is normal after the death of a loved one.
DEPRESSION DSM 5 PROFESSIONAL
As a professional with an MSW, this article causes me to pause and to express concern. Thanks to LinkedIn, I came across an article on Grief/Bereavement and Depression in the NY Times.